Philippines Toolkit: Service Delivery
- Home
- Help and Support
- Close
- Toolkits
- Global Toolkit
- AYSRH Toolkit
- Hub Toolkits
- Core High-Impact Practices
- Gender Essentials Mini Course
- Close
- Resource Collection
- Community of Practice
- Coaching
- Log In/Register
- My Profile
- English
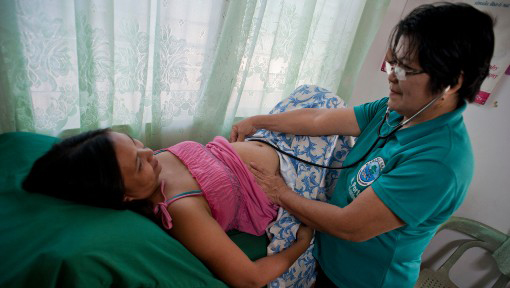
Mobile Outreach Services
 Outreach refers to the provision of health services by trained providers outside traditional health facilities, allowing them to reach populations that may face barriers to accessing facility-based care. By bringing healthcare services directly to communities, outreach efforts aim to bridge gaps in healthcare access and utilization.
Outreach refers to the provision of health services by trained providers outside traditional health facilities, allowing them to reach populations that may face barriers to accessing facility-based care. By bringing healthcare services directly to communities, outreach efforts aim to bridge gaps in healthcare access and utilization.
Mobile Family Planning (FP) Outreach, as outlined in the DOH Guidelines, is a specific approach where FP services are delivered by a trained outreach team in areas characterized by:
- High Unmet Need for FP
- Demand for Long-Acting Reversible Contraceptives (LARCs)
- Inadequate or unavailable trained FP providers
- Infeasibility of establishing fixed service sites
Outreach serves as a crucial tool for expanding access to healthy services, practices or products, typically achieving one or more of the following objectives (excerpt from Community Toolbox):
- Directly delivering health services or products to target populations;
- Educating and informing the target population to increase their knowledge and skills;
- Educating individuals who interact with the target population, such as Community Health Volunteers; and,
- Establishing beneficial connections between individuals and organizations within the community
Mobile outreach services play a vital role in addressing disparities in access to FP services and commodities, thereby assisting women and men in meeting their reproductive health needs. This approach advocates for the delivery of FP services by trained providers outside traditional health facilities, promoting both advocacy and service delivery efforts in the field of FP.
What are the benefits of MOS?
- Outreach enables the flexible and strategic allocation of resources such as healthcare providers, FP commodities, supplies, equipment, vehicles, and infrastructure to areas with the highest need, at intervals that most effectively meet demand.
- Delivering services outside health facilities allows healthcare teams to reach community members who may be hesitant or unable to seek or access healthcare through traditional means.
Outreach as a High-Impact Practice (HIP) in relation to Universal Health Care (UHC)
The MOS HIP approach aims to broaden the reach of FP beyond traditional avenues by extending services beyond Service Delivery Points (SDPs). Recognizing the importance of health equity, this approach acknowledges that certain clients may face barriers in accessing or utilizing FP services through regular channels. These underserved populations require specific attention and outreach efforts.
To expand family planning coverage through outreach, the system must include:
- Health Services: Fully staffed and operational SDPs providing regular in-reach FP services.
- Health Information: Comprehensive health data to identify areas with high client volume and special populations. Additionally, an active client feedback system post-outreach is necessary.
- Leadership: A comprehensive plan for both general and targeted demand generation, focusing on priority populations.
- Health Services: High-quality, accurate, and accessible health information tailored to the needs of the target population.
How to implement
Step 1: Assess the need for outreach
Outreach is a valuable complement to facility-based service delivery (in-reach), extending services to populations who may face barriers to accessing traditional healthcare settings. However, it can be resource-intensive and must be carefully planned and executed. Therefore, it is essential to identify specific populations that may benefit most from outreach efforts.
According to the Western Australia DOH Talk Test Treat Trace Manual, outreach programs should:
- Target priority populations with limited access to services, ensuring resources are allocated effectively;
- Align with the objectives of national and local health strategies;
- Involve thorough planning and engagement with key stakeholders, including community members and health organizations;
- Include evaluation to assess program effectiveness and inform adjustments for ongoing success; and,
- Facilitate access to in-reach services for marginalized groups during follow-up activities.
Step 2: Assess community needs, issues, and resources
Begin by identifying and mapping the catchment areas served by the SDPs offering FP services. Before initiating outreach efforts, consider conducting preliminary information campaigns or surveys to pinpoint areas where outreach is most needed. Focus on identifying regions with:
- Issues related to physical access, such as Geographically Isolated and Disadvantaged Areas (GIDA) or densely populated urban areas.
- Special populations with high demand but limited access, including adolescents, women in the workforce, and sex workers.
- Special populations with traditionally low demand, such as males, specific indigenous or religious groups.
For the supply side, the City Health Office (CHO) must evaluate the SDP responsible for the identified area. Assess the following:
- Adequacy of human resources, including midwife-to-client ratios and Barangay Health Worker (BHW) coverage. Does the SDP have sufficient human resources?
- Facility suitability and availability of FP commodities. Does the SDP have the appropriate facility and adequate supply of commodities?
- Consistency of FP service provision at the SDP. Is the SDP offering FP services regularly as in-reach?
- Existence of mobile outreach efforts for related health programs, like health caravans or door-to-door surveys. Is the SDP currently running any mobile outreaches for other related health programs?
- Presence of existing programs addressing access issues at the health center or barangay level. Are there any programs by the Health center, or Barangay currently
- Addressing the issue with access?
- Availability of support from third-party NGOs or CSOs in the area. Are there any third party NGOs or CSOs in the area that can be tapped to provide support?
- Access to data or resources for post-outreach evaluation at the SDP. Does the SDP have the data or resources to conduct post-outreach evaluation?
Step 3: Identify and prepare outreach sites
- Determine the date and location in collaboration with the Barangay and Health Center responsible for the area. Consider involving schools, tribal leaders, religious leaders, social welfare organizations, and beneficiaries of the 4Ps program.
- Identify the nearest SDP to the outreach location. The SDP in charge of the catchment area should assess its human resource and supply capacity, with additional support provided by the CHO, Barangay, or Civil Society Organizations (CSOs).
- Develop a comprehensive and targeted information campaign tailored to address specific misconceptions or garner support. Utilize materials in the local vernacular whenever possible.
- Conduct door-to-door information campaigns with the assistance of Barangay Health Workers (BHWs) and Barangay Service Point Officers (BSPOs) to identify individuals in need of outreach services.
- Establish a post-outreach monitoring system. Provide clients with a directory or hotline for the nearest health facility and instructions on when to follow up. Additionally, provide the SDP with a list of attendees and their contact numbers for follow-up purposes.
Tip: Ensure all clients receive a directory of the nearest health center with a hotline. Establish communication between the outreach coordinator and the SDP responsible for the catchment area.
Step 4: Capacitate the Health Staff
- Ensure the outreach team comprises the following roles as per the DOH Guidelines on Mobile Outreach:
- Outreach Team Leader
- At least one (1) physician trained in providing Non-Scalpel Vasectomy (NSV), Intrauterine Device (IUD), or Progestin Subdermal Implant (PSI)
- Nurses and midwives certified in Family Planning Competency-Based Training (FPCBT)
- Support staff for triage, anthropometrics, health promotion, and monitoring stations (Community Health Volunteers or non-health staff)
- Driver
- Referral Coordinator at the outreach site
- Referral Coordinator at the nearest SDP based on proximity to the HC
- Ensure all participating healthcare workers receive training in delivering FP services. Conduct refresher orientations covering counseling, pregnancy testing, Responsible Parenthood (RP) education, and referral procedures.
- Tap CHVs to conduct house-to-house mobilizations, distribute flyers, and promote upcoming outreach events.
- Deliver quality FP services during the outreach, including counseling, pregnancy testing, and provision of the client’s chosen FP method, or offer referrals when desired methods are unavailable.
- Record all data in the register of designated facilities for proper documentation and monitoring.
Step 5: Design and Conduct the Outreach
Contrary to common belief, research by Bersamin et al. (2011) and Goodman et al. (2007) consistently indicates that geographic proximity alone does not significantly contribute to teenage pregnancy rates. Instead, barriers to healthcare access often stem from systemic deficiencies or organizational shortcomings. These issues may include inadequate health infrastructure, shortages of commodities, or limited human resources. It is imperative to address these underlying problems before initiating any outreach efforts.
See box below Steps for more on access issues.
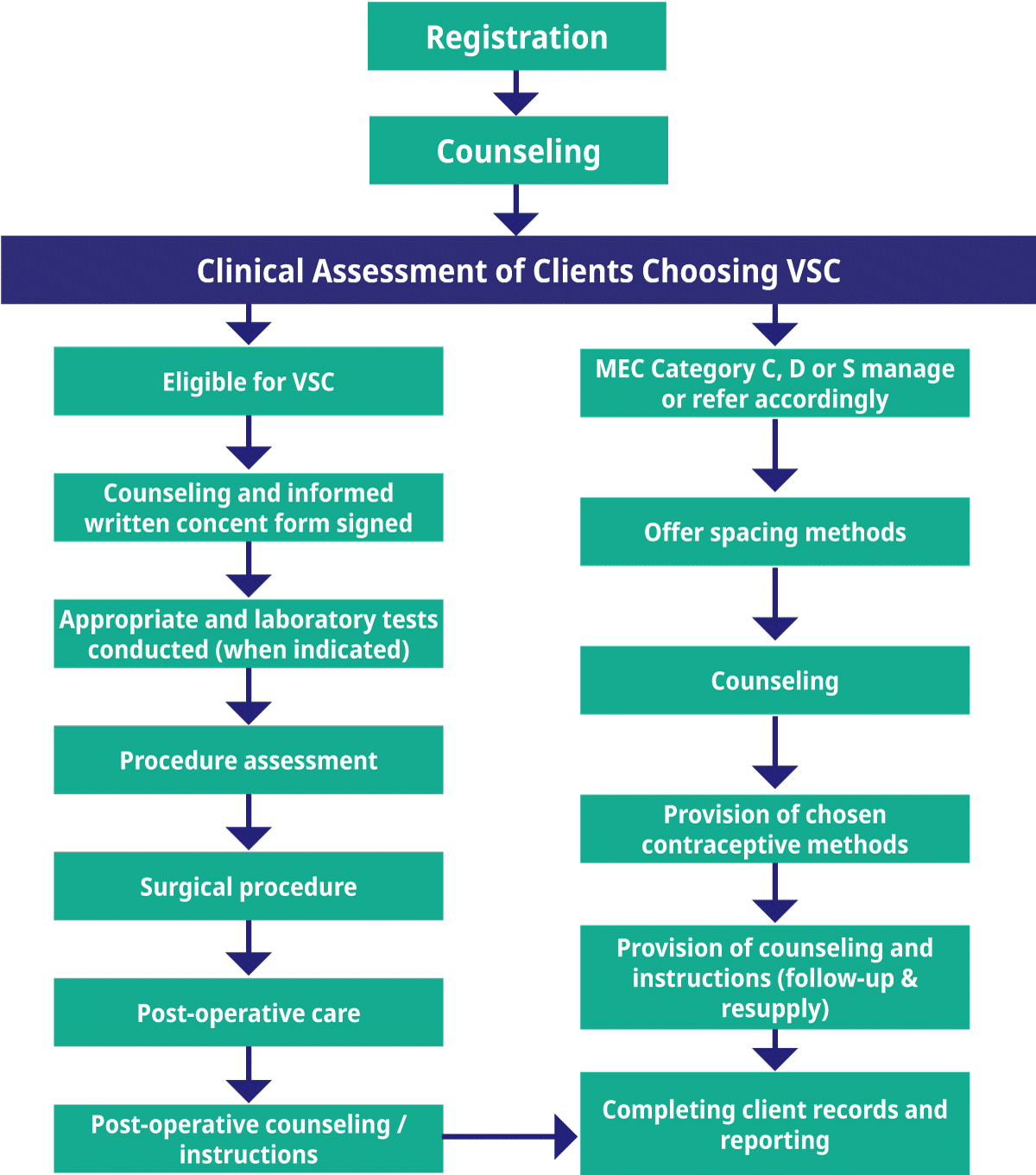
The standard process for conducting outreach typically follows a general pattern, as illustrated in the figure below from the DOH Guidelines on Implementation of Mobile Outreach in Family Planning. This process typically includes stages from triage and initial counseling to the provision of methods.
After the outreach event, it is crucial to follow up with both service providers and clients. Here is how:
- For Clients: Provide information for follow-up and a directory of the nearest health center where they can access further services.
- For the Training Team: Hold a debriefing session to evaluate the activity and gather feedback to inform the planning of future outreach events.
- For the Health Center/SDP: Provide a list of attendees who availed of family planning commodities during the outreach and schedule them for follow-up services.
It is essential to conduct a systemic analysis of outreach activities, following the Quality Implementation Checklist for Mobile Outreach Services, to ensure effectiveness and identify areas for improvement.
Access Issues
Populations facing issues in physical access often encounter barriers when trying to access services. These barriers may arise from residing in remote rural areas or living relatively close to the service center but facing significant time and travel expenses to reach it, especially in urban areas. Outreach activities for these populations typically involve single events conducted away from the service center. During these events, the outreach team selects a specific date and location, often distant from the center, to conduct activities such as outreach caravans or door-to-door visits.
Tip: Filipinos commonly perceive outreach events as one-time occurrences. In addition to the intended purpose of family planning outreach, some individuals may seek assistance for unrelated health issues or attempt to obtain medications outside the planned outreach scope. To address this, the CHO should consider integrating family planning with other health-related services during outreach events or have an emergency response team available to handle emerging health concerns.
Pros:
- Outreach is a straightforward approach that can be conducted independently or as part of other single-day events.
- It often leads to a single point incidence increase in new acceptors of family planning services.
Cons:
- It can be cost-intensive, requiring the establishment of a separate budget for the event.
- Outreach activities are labor-intensive, often necessitating the outsourcing of staff from nearby health centers.
- There may be low sustainability as individuals typically do not follow up with health centers after the outreach event.
It is important to be prepared to accommodate clients who seek consultation for conditions other than family planning. Setting up a medical booth and providing referrals for such cases is essential.
Outreach efforts for these communities need to be tailored to address their specific needs and preferences. This includes:
- Providing information on their preferred FP methods;
- Normalizing the behavior of seeking FP services;
- Promoting non-judgmental and unbiased use of FP; and,
- Emphasizing the importance of follow-up and maintenance of FP methods.
Consequently, outreach activities should be designed to fit the needs and availability of these populations. Some examples of specialized outreach approaches include:
- Extending service hours (sunset clinics) to accommodate individuals busy with work or school, or those who wish to avoid crowded health centers.
- Providing family planning services in the workplace through passive distribution of commodities in company bathrooms, lounges, or common areas, or through sample distribution.
- Organizing special point-of-service delivery events in workplaces or near red-light districts.
It is important to note that the Department of Education (DepED) prohibits the direct provision of FP commodities in schools.
Pros:
- These populations typically have a high demand for family planning services and may already have preferred family planning methods.
- Many of these populations may require long-acting reversible contraceptives (LARCs).
Cons:
- Specialized outreach activities are typically conducted over a set period of time and require continuous coordination with barangay officers, Barangay Health Workers (BHWs), and office managers.
There is a risk that individuals reached through these outreach efforts may not follow up at health centers. It's important to anticipate this by providing LARCs or establishing a referral system.
Populations with traditionally low demand for FP services often have cultural or traditional aversions to family planning. These groups may have been overlooked during outreach efforts due to historical preconceptions, but they still require reproductive services, sometimes even more intensively.
During the preparatory phase of outreach, stakeholders' analysis and Focus Group Discussions are essential to collect supporters and identify misconceptions. Targeted demand generation activities are crucial to dispel myths and align FP with responsible parenthood and traditional values.
Outreach efforts for these populations must be tailored to their specific needs and cultural context. Examples of outreach strategies include:
- Bundling family planning services with other health or government outreach initiatives, such as health service caravans.
- Distributing Information, Education, and Communication (IEC) materials with vouchers for specific FP commodities redeemable at health centers.
- Conducting door-to-door visits to provide FP information, counseling, and direct provision of family planning methods.
Tip: It is important to note that bundling FP services with general health consultations or other services during outreach can help reduce stigma for more "controversial" health services, such as family planning, HIV, or tuberculosis.
Pros:
- Some communities may experience a "domino effect," where even one positive response from an individual can lead to the normalization of FP practices. It's important to identify family planning advocates or champions during outreach events.
Cons:
- Some populations may not consider using FP without the explicit approval of their cultural leaders. Preliminary dialogue with these leaders is essential before conducting outreach.
It is crucial to promote FP without violating the principles of Informed Choice and Voluntarism.
Indicators for success
Vertical Indicators
- Inclusion of MOS into the Program Design
- Inclusion of MOS in the Work & Financial Plan, Annual Operational Plan, Annual Investment Plan
- Adoption of Mobile Outreach standards as per DOH Guidelines on Implementation of Mobile Outreach Services for Family Planning
Horizontal Indicators
- Number of providers trained/oriented on mobile outreaches
- Number of mobile outreaches conducted
What evidence supports the strengthening of family planning through MOS?
In 2023, the City of Manila implemented a successful Bayanihan system of outreach to double its number of FP New Acceptors. The process began with identifying the Top 10 Barangays with the lowest number of new acceptors/current users. Health Centers (HCs) responsible for these areas were then equipped with additional commodities and capacity-building support.
The Health Centers were paired within districts, and an outreach team was designated for each center. Every two weeks, the HCs took turns conducting outreach activities. During these sessions, the non-outreach HC sent its team to support the outreach efforts of the designated HC. Meanwhile, the conducting HC dispatched its CHVs and additional staff to conduct door-to-door FP promotion in the community.
If any clients expressed interest in FP services during the outreach activities, they were promptly educated and counseled on the spot. Subsequently, they were offered the commodity of their choice from the range carried by the outreach team.
TCI APP USERS PLEASE NOTE
You will only receive CERTIFICATES by email – when earning a score above 80% – and will not be able to view or print a certificate PDF from the TCI app.
Test Your Knowledge
Earn a Certificate
Services and Supply Approaches
Challenges
- Conducting an outreach is cost-intensive and diverts essential labor and resources away from in-reach sites, potentially impacting their operations and service delivery capacity.
- It is important to maintain adherence to the principles of Informed Choice and Voluntarism during outreach activities. Ensure that the choice of FP commodity provided to the patient was not coerced or influenced by conditional benefits or pressure from the outreach team.
External Resources
- Community Tool Box Ch23. Modifying Access, Barriers, and opportunities | Section 6. Using Outreach to Increase access
- Outreach programs: planning, implementation and evaluation – Lets Yarn. Government of Western Australia Department of Health
- Does distance matter? Access to family planning clinics and adolescent sexual behaviors. Bersamin M, Todd M, Remer L. 2011
- Geographic access to family planning facilities and the risk of unintended and teenage pregnancy. Goodman DC, Klerman LV, Johnson KA, Chang CH, Marth N. 2007
- Stages of Change Theory. In: StatPearls. Raihan N, Cogburn M. 2024
- DepEd blocks condom distribution in schools | Inquirer News. Barahan, E. M. 2017
- Family Planning Vouchers: A tool to boost contraceptive method access and choice – HIPS