पृष्ठभूमि

एक NURHI डिजाइन बाजार छाता Kwara के केंद्रीय राज्य में Ilorin में एक बाजार में परिवार नियोजन को बढ़ावा देता है । छवि क्रेडिट: Akintunde Akinleye, २०१२ ।
अफ्रीका में सबसे अधिक आबादी वाला देश है, नाइजीरिया शहरी विकास दर ३.७५% है, २.५% की एक समग्र विकास दर की तुलना में, शहरी क्षेत्रों में रहने वाली अपनी आबादी के आधे से अधिक के साथ । गर्भनिरोधक उपयोग आम तौर पर अधिक है और प्रजनन स्तर शहरी क्षेत्रों में कम है, के रूप में ग्रामीण क्षेत्रों की तुलना में । हालांकि, गर्भनिरोधक उपयोग प्रायः सभी शहरी निवासियों के बीच वितरित नहीं किया जाता है; सबूत प्रजनन दर और शहरी धन quintiles के बीच गर्भनिरोधक उपयोग व्यवहार में महत्वपूर्ण असमानता का पता चलता है । नाइजीरिया में, शहरी अमीर की तुलना में प्रजनन दर शहरी गरीबों के बीच अधिक है । ज्ञान और आधुनिक गर्भनिरोधक का उपयोग भी अधिक घरेलू धन के साथ वृद्धि हुई है ।
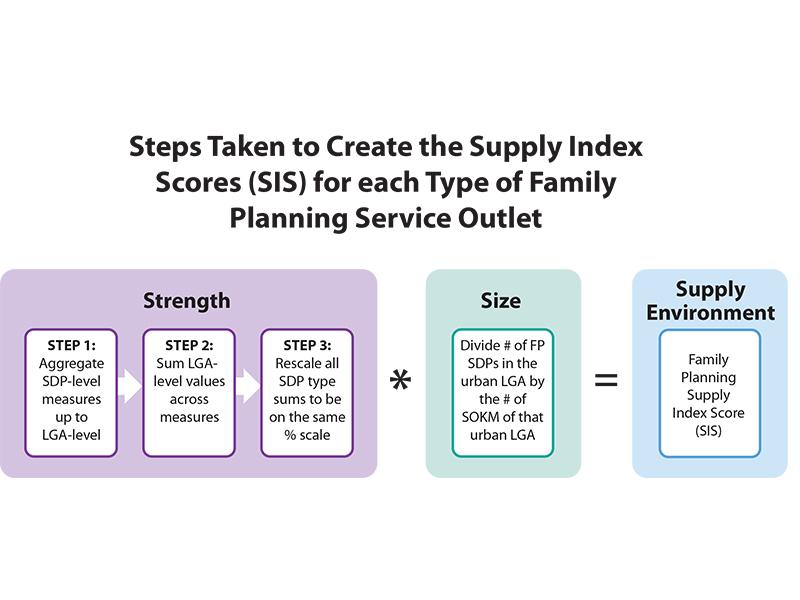
 शहरी क्षेत्रों में सार्वजनिक और निजी दोनों क्षेत्रों में परिवार नियोजन (FP) सेवाओं और आधुनिक गर्भनिरोधक पद्धतियों की उपलब्धता के लिए समान पहुंच सुनिश्चित करना महत्वपूर्ण है । क्योंकि न तो नाइजीरिया में क्षेत्र और धन की स्थिति के विभिंन उपआबादी द्वारा एफ पी सेवाओं की उपलब्धता के उपयोग के बारे में विश्लेषण किया गया था, यह पता नहीं था कि सार्वजनिक या निजी क्षेत्र की सुविधाओं को प्रभावी ढंग से शहरी गरीबों की सेवा कर रहे थे । यह अध्ययन नाइजीरिया के गर्भनिरोधक आपूर्ति वातावरण के बारे में ज्ञान में एक महत्वपूर्ण अंतर भरता है । FP सेवा वितरण बिंदुओं (SDP; इसके बाद सुविधाएं) से सर्वेक्षण डेटा का उपयोग करके, आपूर्ति सूचकांक स्कोर (SIS; इसके बाद स्कोर) में और छह चयनित शहरों में समग्र स्तर के सार्वजनिक और निजी क्षेत्र FP आपूर्ति वातावरण को मापने के लिए बनाए गए थे ।
शहरी क्षेत्रों में सार्वजनिक और निजी दोनों क्षेत्रों में परिवार नियोजन (FP) सेवाओं और आधुनिक गर्भनिरोधक पद्धतियों की उपलब्धता के लिए समान पहुंच सुनिश्चित करना महत्वपूर्ण है । क्योंकि न तो नाइजीरिया में क्षेत्र और धन की स्थिति के विभिंन उपआबादी द्वारा एफ पी सेवाओं की उपलब्धता के उपयोग के बारे में विश्लेषण किया गया था, यह पता नहीं था कि सार्वजनिक या निजी क्षेत्र की सुविधाओं को प्रभावी ढंग से शहरी गरीबों की सेवा कर रहे थे । यह अध्ययन नाइजीरिया के गर्भनिरोधक आपूर्ति वातावरण के बारे में ज्ञान में एक महत्वपूर्ण अंतर भरता है । FP सेवा वितरण बिंदुओं (SDP; इसके बाद सुविधाएं) से सर्वेक्षण डेटा का उपयोग करके, आपूर्ति सूचकांक स्कोर (SIS; इसके बाद स्कोर) में और छह चयनित शहरों में समग्र स्तर के सार्वजनिक और निजी क्षेत्र FP आपूर्ति वातावरण को मापने के लिए बनाए गए थे ।
अध्ययन निंनलिखित मुद्दों को संबोधित किया:
- चाहे सार्वजनिक और निजी क्षेत्र FP आपूर्ति वातावरण शहरी क्षेत्रों में लगातार थे, और यदि नहीं, वे कैसे अलग ।
- अंय क्षेत्र में प्रदान की गई सेवाओं के साथ और एक क्षेत्र में प्रदान की गई सेवाओं को संबद्ध किया गया था या नहीं ।
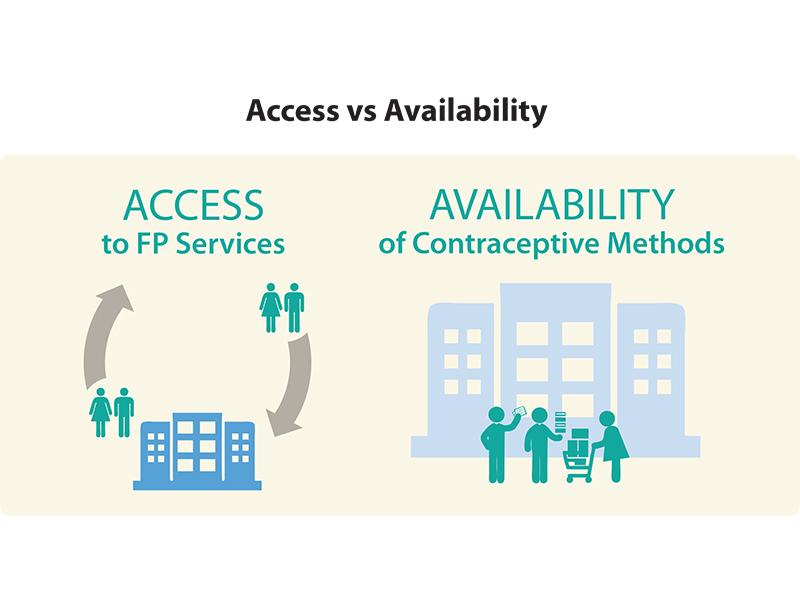
- FP आपूर्ति को उत्पाद की उपलब्धता और गर्भनिरोधक सेवाओं तक पहुंच के रूप में परिभाषित किया गया था । अध्ययन "उपलब्धता" के रूप में माना जाता है कि गर्भनिरोधक वस्तुओं वास्तव में हाथ में थे और किसी भी सुविधा पर प्राप्त किया जा सकता है । "प्रवेश" की डिग्री है जो FP सेवाओं की आबादी का एक बड़ा बहुमत से प्राप्त किया जा सकता है के रूप में परिभाषित किया गया था ।
- इसी समुदायों में रहने वाले व्यक्तियों से एक ही समय में एकत्र डेटा के साथ कुल-स्तरीय सुविधा डेटा को लिंक करके, अध्ययन में पता लगाया कि एफ पी की आपूर्ति पर्यावरण समुदाय स्तर धन की स्थिति के साथ जुड़ा हुआ था, और क्या सेवाओं एक तरीका है कि गर्भनिरोधक का उपयोग और शहरी गरीबों के बीच उपलब्धता के लिए बाधाओं को कम हो सकता है में वितरित किया गया ।
व्यक्तिगत और सुविधा डेटा छह शहरों (अबुजा, बेनिन सिटी, Ibadan, Ilorin, कादुना और Zaria) और 19 स्थानीय सरकारी क्षेत्रों (LGA) से बेसलाइन पर एकत्र किए गए थे । नाइजीरिया राज्यों में विभाजित है, जो LGAs में विभाजित कर रहे हैं । इस अध्ययन में छह चुनिंदा शहरों में झूठ LGAs के शहरी भागों को देखा । १६,१०१ महिलाओं से प्राप्त जानकारी के लिए 19 शहरी क्षेत्रों में साक्षात्कार और १,२२० सुविधाओं से विश्लेषण किया गया । सुविधाओं की चार श्रेणियां शामिल की गईं: (१) सार्वजनिक क्षेत्र की स्वास्थ्य सुविधाएं; (2) पसंदीदा निजी स्वास्थ्य सुविधाएं; (3) निजी फार्मेसियों; और (4) निजी पेटेंट दवा भंडार (PMSs) । सुविधाओं के विभिंन प्रकार के और उंहें नमूना ग्राफिक में वर्णित किया जाता है दृष्टिकोण ।
FP के लिए प्रवेश गर्भनिरोधक तरीकों की सुसंगत और सुविधाजनक उपलब्धता पर आकस्मिक है ।
गर्भनिरोधक का उपयोग और उपलब्धता के दो महत्वपूर्ण घटक कुल स्तर FP आपूर्ति पर्यावरण को परिभाषित करने और आपूर्ति सूचकांक स्कोर का निर्धारण करने के लिए इस्तेमाल किया गया: प्रत्येक LGA में सुविधाओं और सुविधाओं के घनत्व के बीच FP आपूर्ति की समग्र शक्ति जो प्रत्येक क्षेत्र में FP उपलब्ध कराते हैं ।
परिणाम
FP आपूर्ति की शक्ति: विभिंन प्रकार की सुविधाओं के बीच FP आपूर्ति स्कोर की औसत शक्ति कम थी, सार्वजनिक और निजी क्षेत्रों के बीच थोड़ा भिंनता के साथ । इसका तात्पर्य यह है कि प्रत्येक LGA में सुविधाओं का एक पर्याप्त प्रतिशत या तो: (1) सभी गर्भनिरोधक तरीकों कि आम तौर पर सुविधा के प्रत्येक प्रकार में उपलब्ध होना चाहिए की पेशकश नहीं की; (2) अनुभवी कमोडिटी स्टॉक बहिष्कार; (3) प्रति सप्ताह घंटे की अधिकतम संख्या के लिए खुला नहीं थे; (४) सामाजिक रूप से विपणन उत्पादों की पेशकश नहीं की थी; और/या (5) आवश्यक भागीदार सहमति (नहीं नसबंदी सहित) कम से एक उपलब्ध विधि प्राप्त करने के लिए । उदाहरण के लिए, सार्वजनिक और पसंदीदा निजी क्षेत्र सुविधाओं के बीच, अंक बढ़ाने वाले तत्वों की संख्या घंटों की थी, जो सुविधाएं खुली थीं और अंतर्गर्भाशयी डिवाइसेस (आईयूडी) और इंजेक्टेबल को बेचे जाने वाले प्रतिशत थे । सार्वजनिक और पसंदीदा निजी सुविधाओं के लिए कुल स्कोर नीचे लाया गया क्योंकि 19 शहरी क्षेत्रों में से प्रत्येक में एक बड़ा प्रतिशत प्रतिवर्ती आधुनिक गर्भनिरोधक विधियों के लिए आवश्यक साझेदार सहमति ।
औसत पर, सार्वजनिक और पसंदीदा निजी सुविधाओं के ७६.१% के ६०.४% की आवश्यकता साथी सहमति के लिए कम से एक उपलब्ध प्रतिवर्ती गर्भनिरोधक विधि ।
सुविधाओं का घनत्व: यद्यपि वहां सर्वेक्षण क्षेत्रों में कोई प्रत्यक्ष पैटर्न था, फार्मेसियों और PMSs के औसत घनत्व दूर था कि सार्वजनिक और पसंदीदा निजी सुविधाओं के लिए अधिक से अधिक है । इस मामले में, डेटा शहरी LGAs भर में सार्वजनिक और पसंदीदा निजी सुविधाओं के घनत्व में व्यापक परिवर्तनशीलता दिखाई । PMSs का घनत्व है कि गर्भ निरोधकों ले LGAs भर में सबसे अधिक, 100km2 प्रति पीएमएस सुविधाओं की ंयूनतम संख्या के साथ 13 और अधिकतम ४९८ जा रहा है । जहां एक अच्छा सार्वजनिक क्षेत्र fp आपूर्ति पर्यावरण था, वहां की संभावना बढ़ गई थी कि वहां भी एक अच्छा निजी क्षेत्र fp आपूर्ति पर्यावरण था । यह परिणाम सभी स्वास्थ्य सेवाओं के लिए अधिक से अधिक मांग को प्रतिबिंबित और इस प्रकार उन शहरी क्षेत्रों में और अधिक प्रदाताओं सकता है । हालांकि, वहां शहरी LGA जनसंख्या के आकार और प्रदाताओं के घनत्व के बीच एक महत्वपूर्ण सहयोग नहीं था, इसलिए इस खोज की एक और व्याख्या है कि न तो क्षेत्र सेवा वितरण में अंतराल पता काम कर रहा है । इसलिए सरकार ने निजी सुविधाओं की कमी वाले क्षेत्रों में सार्वजनिक FP सुविधाएं बढ़ाई तो आधुनिक गर्भनिरोधकों तक पहुंच में सुधार किया जा सकता है ।
यदि सरकार ने निजी सुविधाओं के अभाव वाले क्षेत्रों में सार्वजनिक FP सुविधाएं बढ़ाई तो आधुनिक गर्भनिरोधकों तक पहुंच में सुधार किया जा सकता है ।
FP आपूर्ति पर्यावरण और सामुदायिक स्तर की धन स्थिति: आंकडे बताते हैं कि सार्वजनिक और निजी क्षेत्र के गर्भनिरोधक उपयोग और उपलब्धता का स्तर प्रत्येक शहर में सबसे गरीब महिलाओं के स्थान से संबद्ध नहीं है. जो लोग गरीब है बस के रूप में एक अच्छा FP आपूर्ति वातावरण में जो धनी है के रूप में रहने की संभावना है, जो शहर में वे रहते है पर निर्भर करता है । इस परिणाम की संभावना इंगित करता है कि FP आपूर्ति वातावरण की जरूरत है कि धन आधारित नहीं है कार्य करता है ।
प्रोग्रामेटिक निहितार्थ

एक पेटेंट दवा विक्रेता, प्रमुख स्टीफन-कोला Adewunmi, उनकी दुकान में एक ग्राहक, Lasisi Iyanda हमेद, सलाह । प्रदर्शन पर नाइजीरियाई शहरी प्रजनन स्वास्थ्य पहल (NURHI) को बढ़ावा देने के सामग्री रहे हैं । छवि क्रेडिट: Akintunde Akinleye, २०१२ ।
यह अध्ययन शक्ति और शहरी नाइजीरिया में निजी और सार्वजनिक FP आपूर्ति के वातावरण के आकार की ध्वनि आधारभूत उपाय प्रदान करता है । यह शहरी क्षेत्रों है कि एक कमजोर आपूर्ति पर्यावरण है और उन क्षेत्रों में जो शहरी गरीबों में स्थित है तुलना दिखाता है । हालांकि कोई व्यवस्थित पैटर्न निजी और सार्वजनिक FP आपूर्ति पर्यावरण और शहरी गरीबी के बीच पाया गया था, कार्यक्रम योजनाकारों और नीति निर्माताओं की जानकारी का उपयोग करने के लिए विशिष्ट भौगोलिक क्षेत्रों और अवसरों की पहचान के लिए निजी क्षेत्र को प्रोत्साहित कर सकते है उच्च केंद्रित गरीब क्षेत्रों में सार्वजनिक सेवाओं का विस्तार और/या पुनर्वितरण करने के लिए और एफ पी की उपलब्धता के लिए खराब पहुंच भी है ।
यह कहानी मूल रूप से द्वारा लिखा गया था माप, सीखना & मूल्यांकन परियोजना, जिसने केन्या, सेनेगल, नाइजीरिया और भारत में शहरी प्रजनन स्वास्थ्य पहल (यूएचआरआई) का मूल्यांकन किया । The Challenge Initiative यूएचआरआई के तहत विकसित सिद्ध समाधानों और सफलताओं तक पहुंच का विस्तार करने का आरोप है।