Emergency contraception (EC) has gained importance in sub-Saharan Africa in the prevention of unwanted pregnancies. Although rates are low, recent Demographic and Health Surveys have documented that EC use is highest in Kenya (1.7%) and Nigeria (2.8%). Studies with small and unrepresentative samples have been conducted in both countries, but they do not provide a full understanding of the characteristics of EC users.
This study provides information from the largest representative sample to date of EC users.
Key research questions included:
- What is the association between EC use and socio-demographic variables?
- What is women’s level of correct knowledge and use of EC?
- What is the association between different behaviors and the use of family planning (FP) or EC methods?
- What is a woman’s preferred source of EC?
 Data were collected as a part of the baseline study of the Urban Reproductive Health Initiative in both Kenya and Nigeria. Data were collected through household surveys from 7,785 sexually experienced women in five cities in Kenya in 2010. In Nigeria, 12,652 sexually experienced women were interviewed in six cities in 2011.
Data were collected as a part of the baseline study of the Urban Reproductive Health Initiative in both Kenya and Nigeria. Data were collected through household surveys from 7,785 sexually experienced women in five cities in Kenya in 2010. In Nigeria, 12,652 sexually experienced women were interviewed in six cities in 2011.
Study Results
- Knowledge of EC was 58% in Kenya and 31% in Nigeria.
- In both countries, never-married sexually experienced women were significantly more likely to be aware of EC than were ever-married women (65% versus 55% in Kenya, and 50% versus 28% in Nigeria).
- 80% percent of Kenyan women who had ever had sex and 52% of Nigerian women reported having used a modern FP method.
- Pharmacies or drug stores were the most common sources for EC (96% in Kenya and 92% in Nigeria).
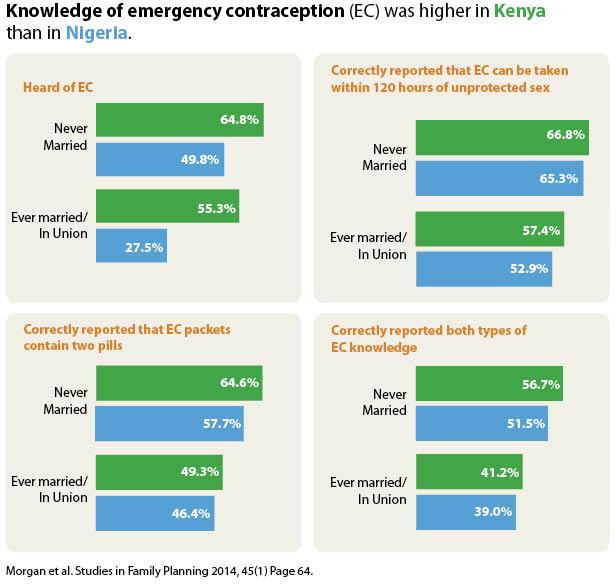 In addition to gauging women’s awareness of EC, the study examined women’s level of correct knowledge of EC use, which was measured by inquiring about (1) knowledge of the number of pills in a dedicated EC product and (2) knowledge of the timeframe after sex within which EC may prevent pregnancy. Among never-married women aged 15 to 49 who had ever had sex and who had ever heard of EC, more than half in both Kenya (57%) and Nigeria (52%) knew that one package of EC includes two pills, and that EC can be taken within 120 hours of unprotected sex. Knowledge of both of these features of EC was significantly lower for ever-married women in both countries (41% in Kenya; 39% in Nigeria).
In addition to gauging women’s awareness of EC, the study examined women’s level of correct knowledge of EC use, which was measured by inquiring about (1) knowledge of the number of pills in a dedicated EC product and (2) knowledge of the timeframe after sex within which EC may prevent pregnancy. Among never-married women aged 15 to 49 who had ever had sex and who had ever heard of EC, more than half in both Kenya (57%) and Nigeria (52%) knew that one package of EC includes two pills, and that EC can be taken within 120 hours of unprotected sex. Knowledge of both of these features of EC was significantly lower for ever-married women in both countries (41% in Kenya; 39% in Nigeria).
Never-married, sexually experienced women in both countries were significantly more likely than were ever married women to have 1) ever used EC, 2) used EC during the past year, and 3) used EC more than once per month at any time during the past year. In both countries, never-married, sexually experienced women were significantly more likely than were ever-married women to consider EC to be their primary method of FP, although these proportions were quite low. Among women who used EC at least once during the past year, 44% in Kenya and 35% in Nigeria reported currently using a non-EC modern method of FP.
 Also of interest was whether women used EC as a regular method of FP. Among Kenyan women who used EC at least once during the past year, 18% reported using EC more than once per month at any time during the past year, and 12% reported that they used EC as their primary method of contraception. Recent users of EC in Nigeria were much more likely than were those in Kenya to use EC regularly (48%) and as a primary method of FP (38%). As to the preferred source of EC among women who had ever used EC, nearly all women in Kenya (96%) and Nigeria (92%) reported that if they needed to obtain EC, they would most likely obtain it from a pharmacy or a drug shop.
Also of interest was whether women used EC as a regular method of FP. Among Kenyan women who used EC at least once during the past year, 18% reported using EC more than once per month at any time during the past year, and 12% reported that they used EC as their primary method of contraception. Recent users of EC in Nigeria were much more likely than were those in Kenya to use EC regularly (48%) and as a primary method of FP (38%). As to the preferred source of EC among women who had ever used EC, nearly all women in Kenya (96%) and Nigeria (92%) reported that if they needed to obtain EC, they would most likely obtain it from a pharmacy or a drug shop.
This large urban study of women and contraceptive use allowed for comparisons between women: 1) who had never used EC; 2) have used EC but not during the year prior to the study; and 3) who have used EC in the past year. In both Nigeria and Kenya, recent and past EC users were generally in their twenties. A greater proportion had a secondary or higher level of education. In Nigeria, religious affiliation was associated with EC use; this was not the case in Kenya. In both countries, marital status was inversely correlated with EC use; those who were never married were significantly more likely than those who were ever married to have used EC. In addition, in both countries, those who had at least one child were more likely to have never used EC (roughly 80%) than to have used non-recently (approximately 65%) or recently (roughly 51%). Recent users in Kenya and both recent and non-recent users in Nigeria were more likely to report having more than one sexual partner in the past year.
In both countries, marital status was inversely correlated with EC use; those who were never married were significantly more likely than those who were ever married to have used EC.
Programmatic Implications
This study deepens the understanding of when, how, and by whom EC are used in urban Kenya and Nigeria. The findings counter the public perception in these countries that adolescents are the primary users of EC. Instead, the data confirm the findings of previous studies that the majority of users in urban areas are in their twenties, educated, employed, and unmarried. The findings also refute the presumed association between EC use and sexual-risk taking. The results indicate the important role the private sector plays in delivering FP services that are not dependent on a provider.
 One surprising finding is the relatively high proportion of women in Nigeria who identify EC as their primary method of FP. This result likely reflects a response to the more limited access and use of other contraceptive options in Nigeria, where far fewer urban women have ever practiced modern contraception. The Nigerian women may be using the more readily available EC as a replacement for the more difficult to obtain or less familiar FP methods.
One surprising finding is the relatively high proportion of women in Nigeria who identify EC as their primary method of FP. This result likely reflects a response to the more limited access and use of other contraceptive options in Nigeria, where far fewer urban women have ever practiced modern contraception. The Nigerian women may be using the more readily available EC as a replacement for the more difficult to obtain or less familiar FP methods.
The high proportion of recent EC users who report using EC more than once per month and as a primary method of contraception (particularly in Nigeria) indicate the need for greater understanding of the dynamics of repeated use and the importance of ensuring the availability of and access to effective, short-term, women-controlled barrier and hormonal methods. Also highlighted by the study is the need to adequately target information and services about EC to unmarried urban women. Although the private sector is well placed to ensure service availability, the public sector and civil society should complement these efforts through activities that raise awareness. Social marketing initiatives that provide poorer women access to subsidized EC pills at a lower cost than commercially available EC are also important in contexts where price may be a barrier for poorer women.
This story was originally written by the Measurement, Learning & Evaluation Project, which evaluated the Urban Reproductive Health Initiatives (UHRIs) in Kenya, Senegal, Nigeria and India. The Challenge Initiative is charged with expanding access to the proven solutions and successes developed under the UHRIs.


